Ivermectin is commonly used as a parasiticide in many species of animals. For dogs, the medication is typically prescribed as a heartworm preventive; microfilaricide (i.e., to kill immature heartworm larvae in a dog’s bloodstream); treatment for sarcoptic and demodectic mange and ear mites; and for certain relatively rare types of internal parasites. When used at the right dose in the right patient, ivermectin is very safe, but when misused or in cases of accidental overexposures, ivermectin toxicosis can be fatal. Knowing how and when to use ivermectin, and just as importantly, when not to use it, is essential to preventing illness and death in dogs.
Appropriate Dosing
Ivermectin is used at different doses for various uses. Examples in dogs include:
The dose of 6 ug/kg prescribed for heartworm prevention is exceptionally low and safe for all dogs. However, higher doses can have serious adverse effects in some individuals and should never be given to a dog except under the direct supervision of a veterinarian.
Toxic Levels and the Gene for Multidrug Resistance
Most dogs need to be exposed to more than 2000 ug/kg of ivermectin before significant symptoms of an overdose develop, but this is not true for all individuals. Some dogs carry a genetic mutation called ABCB1 (previously known as MDR1) that make them especially sensitive to ivermectin and some other medications including moxidectin, loperamide, mibemycin, and some types of chemotherapies. The potentially toxic dose of ivermectin in an ABCB1 positive dog can be as low as 100ug/kg.
Herding breeds and associated mixed-breed dogs are at highest risk for being affected by the ABCB1 gene. These include Collies, Shetland Sheepdogs (Shelties), Australian Shepherds, Old English Sheepdogs, English Shepherds, German Shepherds, Long-haired Whippets, and Silken Windhounds. Whenever doubt exists as to whether ivermectin or any drug linked to problems with the ABCB1 gene might prove dangerous to a particular dog that individual should undergo genetic testing before being treated. In the United States, a veterinarian or pet owner can collect cells via a cheek swab or a blood draw and send the sample to Washington State University’s Veterinary Clinical Pharmacology Laboratory for analysis.
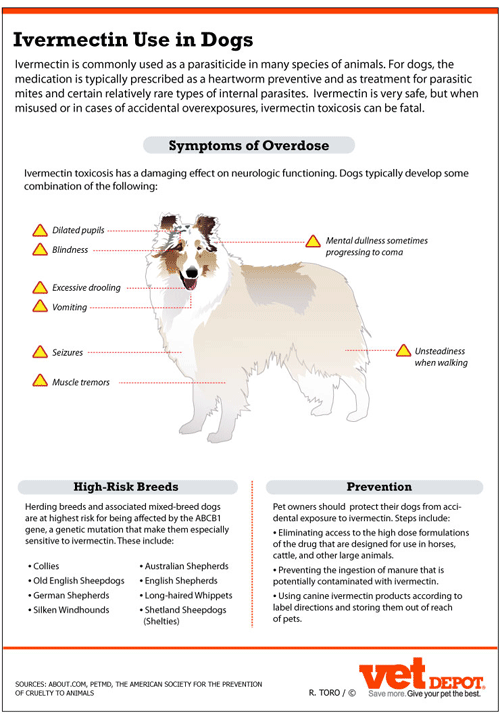
Symptoms of an Overdose
Animals can absorb toxic levels of ivermectin through oral ingestion, topical exposure, or injection. Dogs that live on or visit farms and ranches are at especially high risk for ivermectin poisoning because they may have access to high-dose formulations of ivermectin intended for use in horses, cattle, and other large animals. It is also possible for dogs to ingest enough ivermectin in the feces of another animal (e.g., horse or cattle manure) to make them ill.
The symptoms of ivermectin toxicosis develop when the drug crosses the blood-brain barrier and has a deleterious effect on neurologic functioning. Dogs typically develop some combination of the following:
- dilated pupils
- blindness
- unsteadiness when walking
- mental dullness sometimes progressing to coma
- excessive drooling
- vomiting
- muscle tremors
- seizures
Treating Ivermectin Overdoses

If a dog is topically exposed to potentially toxic levels of ivermectin, it should be immediately washed with a mild shampoo or dishwashing detergent and rinsed with copious amounts of cool water. For oral exposures that are caught within four hours, inducing vomiting can expel a significant amount of ivermectin before it is absorbed into the bloodstream. Up to 36 hours after ingestion, the repeated administration of activated charcoal aids in the elimination of the drug from the body.
Treatment for ivermectin toxicosis in dogs is primarily symptomatic and supportive, which gives the body time to eliminate the drug. Intravenous fluid therapy is instituted to maintain adequate hydration in patients that cannot drink. If a dog is unable to safely eat for more than a few days, a feeding tube and nutritional support will be necessary. In less severe cases, the drug physostigmine can be used to temporarily improve a dog’s neurologic status and allow it to take in food.
When dogs cannot breathe adequately on their own, endotracheal intubation and mechanical ventilation should be instituted. This often necessitates referral to a 24 hour veterinary hospital. Intensive nursing care including frequent changes of body position, application of eye lubricants when the blink reflex is absent, and assistance with urination and defecation may also be required. If seizures develop, dogs will need to receive medications to lessen their severity and frequency. Intravenous lipid emulsion therapy is a relatively new but promising option for ivermectin poisoning that might be considered in some dogs.
Prognosis and Prevention
In all but the most severe cases, dogs that have been exposed to a toxic amount of ivermectin can be saved. This is especially true if the animals receive rapid veterinary care and can benefit from decontamination procedures. When large amounts of the medication have been absorbed into the pet’s bloodstream, it can take weeks for a pet to fully recover, and in some cases the cost of aggressive and prolonged treatment results in a decision to euthanize.
Pet owners should take care to protect their dogs from accidental exposure to potentially toxic amounts of ivermectin by:
- eliminating access to the high dose formulations of the drug that are designed for use in large animals except under direct supervision of a veterinarian
- preventing the ingestion of manure that is potentially contaminated with ivermectin
- using canine ivermectin products according to label directions and storing them out of reach of pets
Read more dog poison prevention and safety tips at VetDepot.
Sources
Ivermectin Toxicosis in Dogs. Odunayo A, Kerl M. Clinician’s Brief. 2012 Dec; 63-66.
Intravenous fat emulsion as treatment for ivermectin toxicosis in three dogs homozygous for the ABCB1-1? gene mutation. Wright HM, Chen AV, Talcott PA, Poppenga RH, Mealey KL. J Vet Emerg Crit Care (San Antonio). 2011 Dec;21(6):666-72.
Ivermectin toxicosis in dogs: a retrospective study. Merola V, Khan S, Gwaltney-Brant S. J Am Anim Hosp Assoc. 2009 May-Jun;45(3):106-11