Arthritis (more correctly called degenerative joint disease or osteoarthritis) is very common in companion animals. The disease is an often overlooked cause of what many consider to be normal changes related to the aging process in cats. Because therapeutic options are more limited in comparison to what is available for dogs, cat owners need to be especially alert for the signs of early arthritis in their pets so that treatment can begin when it is most effective.
What is Arthritis?
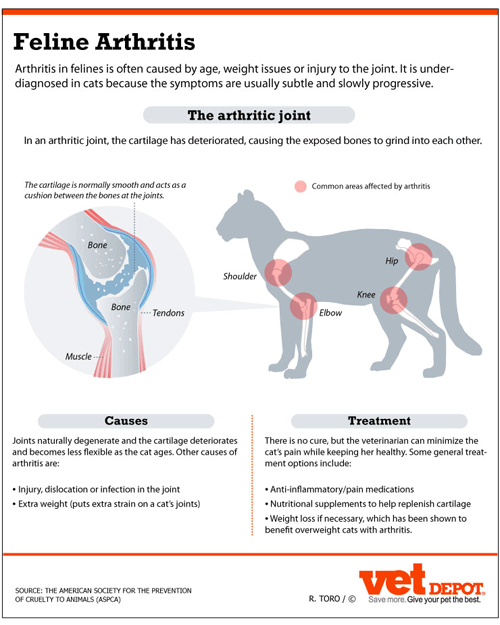
The word “arthritis” simply means “inflammation of a joint,” but veterinarians and owners most often use the term to refer to chronic changes that occur in and around joints as a result of wear and tear produced by advanced age, injury, or developmental disorders. Whatever the cause, arthritis results in the breakdown of cartilage within the joint, a decrease in the protective nature of joint (synovial) fluid, and eventually bony growths around the joint as the body attempts to restrict its movement.
The Symptoms of Arthritis in Cats
Arthritis is under-diagnosed in cats. One study1 revealed that 90% of cats over the age of twelve have evidence of degenerative joint disease on x-rays. Most cats are never diagnosed with arthritis because the clinical signs associated with the feline form of the disease are primarily behavioral. For example:
- Cats may stop grooming themselves, particularly around the lower back due to decreased flexibility.
- They can have difficulty rising, climbing and jumping. As a result, they may no longer frequent their favorite perches or resting places.
- Affected cats often become grumpy, less sociable and playful, and resist being picked up.
- Arthritic cats can have urinary or fecal accidents because of difficulty getting to the litter box, in and out of it, or assuming the posture needed for elimination.
- They may eat less because getting to and eating from a bowl hurts, which can result in weight loss.
- Inactivity causes a loss of muscle mass.
- In some cases, affected cats are noticeably stiff and sore and may limp if one leg if it is affected to a greater extent than others.
These symptoms are usually subtle and slowly progressive, making them difficult for owners to appreciate at home. Unfortunately, cats are even better at hiding their pain while at the veterinary clinic, so doctors also often underestimate the extent of their patient’s discomfort. A thorough physical and orthopedic exam followed by x-rays is needed to definitively diagnose most cases of feline arthritis.
Treating Arthritis in Cats
Nonsteroidal anti-inflammatories (NSAIDs) play a central role in the treatment of arthritis in dogs, but they must be used with caution in feline patients because cats are very sensitive to their side-effects. The repeated use of the NSAID meloxicam (Metacam) has been associated with acute kidney failure in cats. However, some studies have shown that low doses can be used safely over the long-term and may even slow the progression of chronic kidney disease in cats.3 Other medications like buprenorphine, tramadol, amantidine, gabapentin, and corticosteroids (e.g., prednisolone) have all been used to improve patient comfort in cats with arthritis.

Nutritional supplements also have a widely recognized role in the treatment of arthritis in cats. Research has shown that a diet supplemented with eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA)(e.g., salmon oil or Welactin), green-lipped mussel extract (e.g., Glyco-Flex) , and glucosamine/chondroitin sulfate (e.g., Cosequin) improved the mobility of cats suffering from degenerative joint disease.5 These oral supplements are easily added to a cat’s food, but if after trying several different products for eight to nine weeks each they seem ineffective, switching to an injectable polysulfated glycosaminoglycan (e.g., Adequan) is a good option.
Many cats suffering from arthritis benefit from physical therapy and complementary remedies like massage, cold laser treatments, and acupuncture. Combinations of different types of treatment, for example using Cosequin and acupuncture for maintenance therapy and meloxicam on especially bad days, often proves more effective than does any single therapy alone.
Overweight cats should be put on a diet. Excess weight makes getting around on arthritic joints even more painful than it has to be and contributes to their continued break-down. In general, the combination of an appropriate amount of a high protein/low carbohydrate food with suitable exercise is the best way to encourage weight loss and to promote the strong muscles, tendons, and ligaments that help support arthritic joints.
Environmental modifications are an important part of improving and maintaining an arthritic cat’s quality of life. Aspects to consider include:
- a bed that is well-padded, warm, and protected against drafts
- easy access to a low-sided litter box
- easy access to food and water. Raising the bowls so that cats don’t have to flex to eat and drink can be helpful.
- non-slip ramps to favorite perches and resting places
In severe cases, surgery to repair, remove, or replace a severely damaged joint and/or stem cell therapy can be considered.
Prognosis
Arthritis is a progressive disease and as such, treatment plans usually need to be modified as a cat’s condition worsens over time. Nevertheless, with dedicated care most arthritic cats can be expected to enjoy an excellent quality of life for many years after their diagnosis.
Sources
1. Radiographic evidence of degenerative joint disease in geriatric cats: 100 cases (1994–1997). Hardie E, Roe S, Martin F. J Am Vet Med Assoc. 2002 Mar 1;220(5):628-32.
2. Osteoarthritis in the cat: 1. how common is it and how easy to recognize? Bennett D, Zainal Ariffin SM, Johnston P. J Feline Med Surg. 2012 Jan;14(1):65-75.
3. Osteoarthritis in the cat: 2. how should it be managed and treated? Bennett D, Zainal Ariffin SM, Johnston P. J Feline Med Surg. 2012 Jan;14(1):76-84.
4. Diagnosis and treatment of osteoarthritis. Rychel JK. Top Companion Anim Med. 2010 Feb;25(1):20-5.
5. Evaluation of a therapeutic diet for feline degenerative joint disease. Lascelles BD, DePuy V, Thomson A, Hansen B, Marcellin-Little DJ, Biourge V, Bauer JE. J Vet Intern Med. 2010 May-Jun;24(3):487-95. Epub 2010 Mar 22.
The above is provided for information purposes only and should not be used for the diagnosis or treatment of any condition.
This information does not cover all possible variables, conditions, reactions, or risks relating to any topic, medication, or product and should not
be considered complete. Certain products or medications may have risks and you should always consult your local veterinarian concerning the treatment of
your pet. Any trademarks are the property of their respective owners.