The kidneys play many roles in the body. They produce urine by filtering waste products and excess water out of the blood. They also help regulate hydration and electrolyte levels, control blood pressure, and produce a hormone that stimulates red blood cell production. Chronic kidney disease (CKD) develops over time as the kidneys gradually lose their ability to perform these functions.
"Chronic Kidney Disease is a leading cause of death in older dogs and cats."
When healthy, each of an animal’s two kidneys is made up of tens of thousands of nephrons, far more than is needed at any one time. Nephrons do the work of the kidneys but can be damaged and destroyed by infections, toxins (e.g., antifreeze), episodes of low blood pressure, and normal wear and tear. Some individuals may be born with fewer nephrons than normal. When pets lose a large number of nephrons through some combination of these processes, they eventually develop symptoms of chronic kidney disease.
Less severe CKD may be called kidney insufficiency. The terms kidney or renal failure are sometimes used to describe the condition when it is very advanced. Whatever the name used, CKD is a leading cause of death in older dogs and cats.
Diagnosing Chronic Kidney Disease in Cats and Dogs
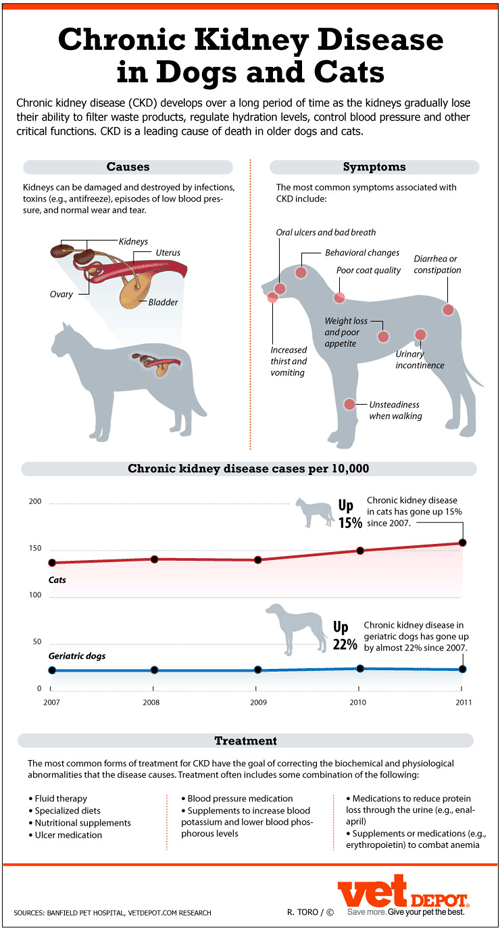
Chronic kidney disease develops over a long period of time. Early in its course, pets appear perfectly normal because of the kidneys’ supply of “extra” nephrons. Once an individual is down to one-third the normal number of nephrons, the kidneys lose their ability to concentrate urine effectively. When only one-quarter of the nephrons remain, abnormalities in blood work develop.
The metabolic waste products blood urea nitrogen (BUN) and creatinine eventually start to build up in the blood instead of being eliminated from the body in the urine. Blood phosphorous levels may increase, and blood potassium levels decline. Affected dogs and cats become dehydrated because of the kidneys’ inability to keep water within the blood stream, allowing it to exit the body in the form of large amounts of dilute urine. Blood pressure can rise, and the kidneys eventually stop producing enough erythropoietin, the hormone that stimulates red blood cell production. This causes affected pets to become anemic.
The most common symptoms associated with CKD include:
- dehydration
- increased thirst and urination
- urinary incontinence
- poor appetite
- lethargy and depression
- behavioral changes
- weight loss and muscle wasting
- vomiting with or without blood
- diarrhea or constipation (stool may be dark and tarry, indicating bleeding within gastrointestinal tract)
- oral ulcers
- bad breath
- poor coat quality
- unsteadiness when walking
Late in the course of the disease, pets may also develop decreased water intake and urination, inability to rise, difficulty breathing, blindness, seizures, and abnormal bruising or bleeding.

CKD can usually be diagnosed based on the results of a blood chemistry panel, complete blood cell count (CBC), and a urinalysis. Characteristically, these tests reveal a low urine specific gravity (dilute urine), high BUN and creatinine levels in the blood, and sometimes anemia and high blood phosphorous and low blood potassium levels. Veterinarians will also typically culture a sample of urine to rule out a urinary tract infection, which can develop as a result of CKD and exacerbate a pet’s symptoms. Patients should also have their blood pressure taken. Additional testing may be necessary based on the dog or cat’s particular situation.
Treating Chronic Kidney Disease
The most common forms of treatment for CKD have the goal of correcting the biochemical and physiological abnormalities that the disease causes. Hospitalization may be necessary at the onset to correct severe dehydration and electrolyte abnormalities and to get patients feeling good enough to go home for maintenance therapy. Treatment often includes some combination of
- Fluid therapy
- Special diets that contain moderate amounts of high quality protein to ease the work of the kidneys while maintaining the pet’s weight and muscle mass. Kidney diets are also low in phosphorous and sodium and high in potassium, B-vitamins, and omega 3 fatty acids. Canned formulations are typically recommended because of their increased water content and palatability.
- Nutritional supplements that support kidney function (e.g., Azodyl and Epakitin)
- Medications to treat or prevent gastrointestinal ulcers (e.g., cimetidine and sucralfate)
- Blood pressure medications (e.g., amlodipine and enalapril)
- Supplements to increase blood potassium and lower blood phosphorous levels
- Medications to reduce protein loss through the urine (e.g., enalapril)
- Supplements like Renal Advanced or medications (e.g., erythropoietin) to combat anemia
New treatments can be an option for owners who are willing and able to pursue advanced therapies. Hemodialysis is available at some referral hospitals but must be administered several times a week. Kidney transplants may be an option for individuals that meet certain criteria. Stem cell therapy is currently under investigation and may prove to be a great leap forward in the treatment of CKD.

Whichever treatment protocol is utilized, owners and veterinarians must stay in close contact with one another to ensure that changes in a pet’s condition are addressed before they can have a significant adverse effect on its quality of life.
Prognosis for Chronic Kidney Disease
CKD is a progressive disease, but the rate at which a pet’s health will deteriorate varies markedly. Some patients can maintain an excellent quality of life for long periods of time with only minor alterations in their care while others rapidly deteriorate with even the most aggressive treatment. In the end, euthanasia is often required once a pet’s suffering cannot be relieved in any other manner.
Sources
Bartges JW. Chronic kidney disease in dogs and cats. Vet Clin North Am Small Anim Pract. 2012 Jul;42(4):669-92, vi.
Polzin DJ. Evidence-based step-wise approach to managing chronic kidney disease in dogs and cats. J Vet Emerg Crit Care (San Antonio). 2013 Mar;23(2):205-15.
Quimby JM, Webb TL, Gibbons DS, Dow SW. Evaluation of intrarenal mesenchymal stem cell injection for treatment of chronic kidney disease in cats: a pilot study. J Feline Med Surg. 2011 Jun;13(6):418-26.
Schmiedt CW, Holzman G, Schwarz T, McAnulty JF. Survival, complications, and analysis of risk factors after renal transplantation in cats. Vet Surg. 2008 Oct;37(7):683-95.